TABLE OF CONTENT

AI in healthcare is no longer a pilot project it's deployed in operating rooms, pathology labs, ophthalmology clinics, and wound care centers across the United States. From detecting malaria in a blood smear to predicting sepsis six hours before standard protocols would flag it, AI Healthcare Solutions are generating measurable, auditable clinical outcomes that hospital administrators and clinical directors can act on today.
This guide documents 7 high-impact AI use cases each with real numbers, verified case studies, and clear commercial value. Whether you are evaluating vendors, scoping an AI pilot, or building a business case for your board, this is the resource that cuts through the noise.
NeuraMonks has delivered production AI systems across pathology, ophthalmology, orthodontics, and wound care. Every case study below reflects work we have shipped not theoretical capability.
1. AI-Powered Blood Cell Analysis & Malaria Detection
Manual blood smear analysis creates a dangerous bottleneck in high-volume diagnostic labs. Skilled technicians spend hours counting and classifying cells work that introduces inter-observer variability and fatigue related errors. In malaria-endemic regions and underserved U.S. communities, a missed positive is not a data point. It is a patient outcome.
How AI Healthcare Solutions Eliminate This Bottleneck
Deep learning models trained on annotated blood smear images automatically segment and classify red blood cells, white blood cells, and platelets at scale. A specialized malaria detection module identifies Plasmodium infected cells with accuracy that matches expert pathologists without fatigue, without variability, and at a fraction of the time.

Key Capabilities
- Automated detection and classification of RBCs, WBCs, and platelets
- Specialized Plasmodium parasite detection module for malaria screening
- End-to-end automation from image ingestion through structured reporting
- Scalable model architecture deployable across multi-site lab networks
- Built on Python + PyTorch with Django-based deployment infrastructure
CASE STUDY
AI Powered Blood Cell & Malaria Detection Improves Diagnostic Accuracy by 35% and Cuts Lab Workload by 55%
See the full case study at NeuraMonks
For high volume labs and hospital pathology departments, this automation directly reduces per sample cost, accelerates patient turnaround, and builds a defensible audit trail for every diagnostic decision.
Stop Planning AI.
Start Profiting From It.
Every day without intelligent automation costs you revenue, market share, and momentum. Get a custom AI roadmap with clear value projections and measurable returns for your business.

2. Automated Wound Detection & Measurement Using Deep Learning
Wound care documentation is one of the most paper-heavy, inconsistent processes in clinical practice. Nurses and wound care specialists measure wounds with rulers, describe them in free text, and photograph them without a standardized protocol. Two clinicians assessing the same wound can produce materially different records which creates compliance risk, billing exposure, and treatment inconsistencies.
What the AI System Does
A deep learning computer vision system automatically detects wound boundaries in clinical photographs, measures area and perimeter, classifies wound type and stage, and generates a structured record that integrates with EHR systems. Every assessment is timestamped, consistent, and comparable across visits giving care teams an objective healing trajectory.

Clinical and Financial Impact
- Eliminates inter-clinician variability in wound staging and measurement
- Enables objective tracking of healing rates to guide treatment escalation decisions
- Supports telehealth wound monitoring patients photograph wounds at home
- Reduces litigation risk through standardized, timestamped documentation
- Integrates with EMR/EHR platforms for seamless workflow adoption
CASE STUDY
Delivered Clinically Accurate Wound Measurements — Reduced Manual Assessment Effort by 60%
See the full case study at NeuraMonks
High value settings: long-term care facilities, burn centers, diabetic wound clinics, and home health agencies all high cost environments where standardized documentation reduces both clinical and administrative burden.
3. AI-Powered Automation in Clinical & Administrative Workflows
Beyond diagnostic imaging, healthcare organizations are deploying AI to automate the administrative and operational processes that consume clinical staff time without adding patient value scheduling, eligibility verification, prior authorization, and internal task routing.
Documented Results from a Real Deployment
A healthcare automation engagement delivered measurable efficiency gains across clinical scheduling and internal workflow management cutting manual processing time, reducing error rates, and freeing clinical staff to focus on patient-facing work.

Automation Capabilities Delivered
- AI-driven scheduling and patient intake routing
- Automated prior authorization data collection and submission
- Internal workflow orchestration with rule-based exception handling
- Real-time dashboard for task status and bottleneck visibility
- Integration with existing EMR and practice management systems
CASE STUDY
AAL Healthcare Automation Efficiency Gains Across Clinical and Administrative Workflows
See the full case study at NeuraMonks
4. Automated Detection of Dental Bite Problems from 3D Scans
Orthodontic diagnosis relies on manual inspection of 3D dental models a process that is slow, experience-dependent, and particularly challenging when a patient presents with multiple overlapping conditions simultaneously. A Class II malocclusion combined with a deep bite and scissors bite is common in complex cases, yet diagnosing all three conditions consistently requires significant clinical experience.
Specialized AI Solutions for Orthodontics
A ResNet 50 based CNN processes 3D dental scan files (STL format), automatically classifying the primary occlusion type and any co existing bite problems. The system delivers ranked predictions with confidence scores and validates all combinations against medical plausibility rules before surfacing results to the clinician.

System Architecture
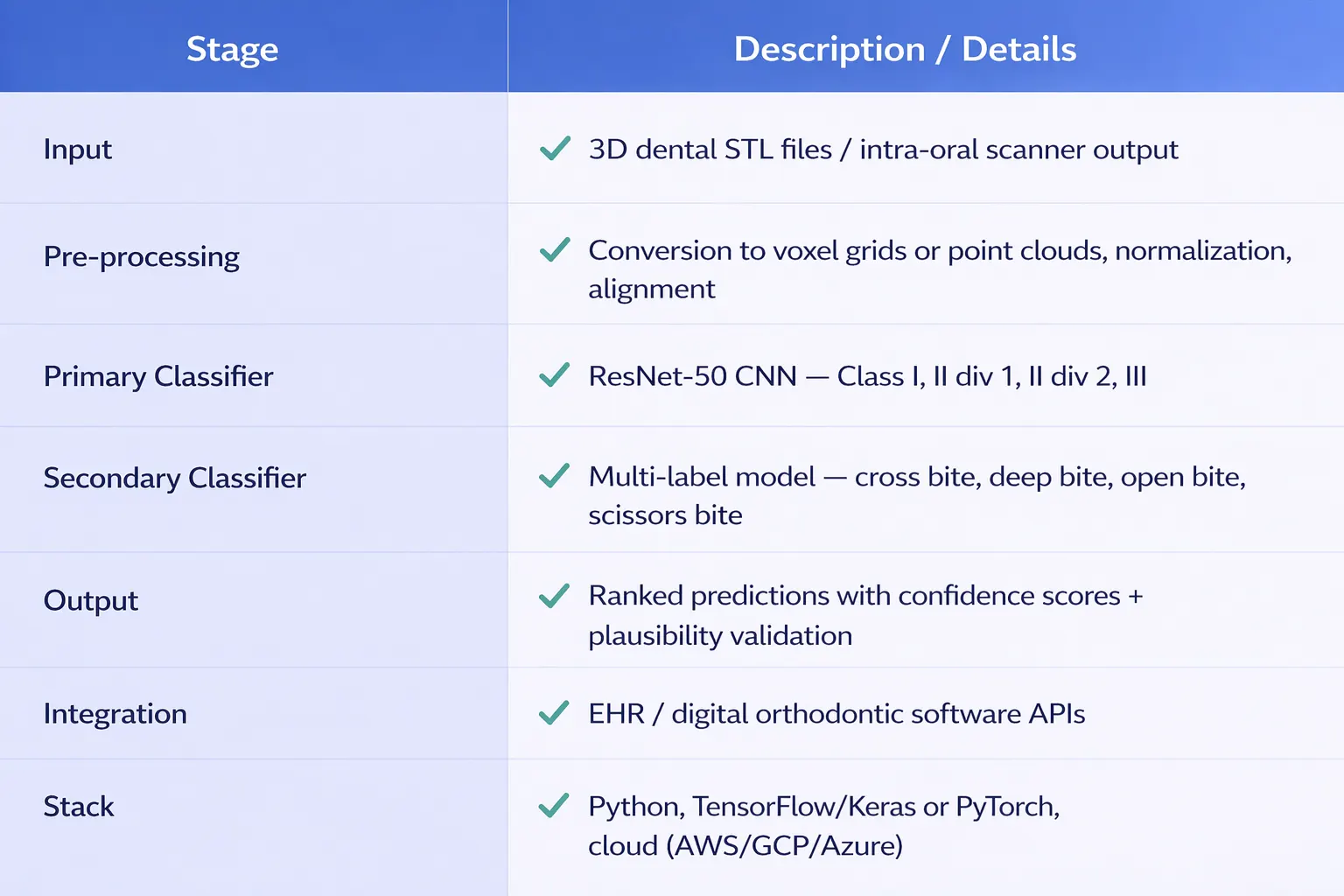
With a Cohen's kappa of 0.86, this system reaches near-expert diagnostic agreement. For orthodontic groups, DSOs, and dental school clinics processing high volumes of new patients, this represents significant time savings and a measurable improvement in diagnostic consistency.
5. AI Clinical Decision Support for Glaucoma Management
Glaucoma affects over 3 million Americans and is a leading cause of irreversible blindness yet up to 50% of cases remain undiagnosed. The disease progresses silently, and staging decisions depend on synthesizing complex variables across a patient's full visit history. When a patient has 80+ recorded visits, manually extracting meaningful longitudinal signal at scale is unrealistic.
Dual-Agent AI Architecture
A multi-agent AI platform processes patient data symptoms, intraocular pressure history, age, optic nerve imaging, visit records against a large repository of historical cases. A Diagnostic Agent generates recommendations, then a separate Validation Agent independently scores them for reliability (0 to 10) before presenting results. The system never forces a conclusion on edge cases low-confidence profiles trigger a direct clinician review flag.


For ophthalmology practices managing large patient panels, this system reduces the cognitive load of routine staging decisions while maintaining human oversight on ambiguous cases.
6. AI-Assisted Radiology: Second-Read Accuracy at Scale
Radiologists in the U.S. read an average of 20,000+ images annually. Imaging volumes are rising while radiologist supply is projected to fall short of demand by 42,000 physicians by 2033. The combination creates conditions for fatigue-related errors particularly for subtle findings like small pulmonary nodules, hairline fractures, or early-stage tumors.
How the AI Functions as a Second Reader
AI radiology tools apply deep learning to X-rays, CT scans, and MRIs to flag anomalies, pre-annotate findings, and prioritize worklists so critical cases surface first. These systems do not replace radiologists they reduce the probability that a clinically significant finding is missed on a high-volume day.

- Faster turnaround times improve patient throughput and revenue per scanner
- Prioritized worklists reduce time-to-treatment for critical findings stroke, PE, pneumothorax
- Documented AI second-read can reduce malpractice exposure
- Scalable across teleradiology networks one AI-augmented radiologist covers more sites
7. Predictive Analytics for Early Sepsis Warning
Sepsis kills approximately 270,000 Americans every year. The condition can progress from a manageable infection to multi-organ failure within hours, and early intervention is the single biggest determinant of survival. Yet hospitals still largely depend on reactive vital sign thresholds and manual escalation protocols.
Continuous Risk Scoring from EHR Data
Predictive AI models analyze EHR data streams in real time vital signs, lab results, medication administration, nursing notes generating sepsis risk scores per patient every few minutes. When a score crosses a defined threshold, the system automatically alerts the clinical team, enabling intervention hours before traditional early-warning scores would trigger.

- Reduced CMS sepsis-related penalties under the Hospital Readmissions Reduction Program
- Improved HCAHPS scores and CMS star ratings directly tied to reimbursement
- Lower cost per sepsis case average ICU sepsis treatment: $25,000–$100,000
- Actionable alerts integrated into existing EHR workflows (Epic, Cerner, etc.)
- Explainable AI outputs clinicians see exactly which data points triggered the alert
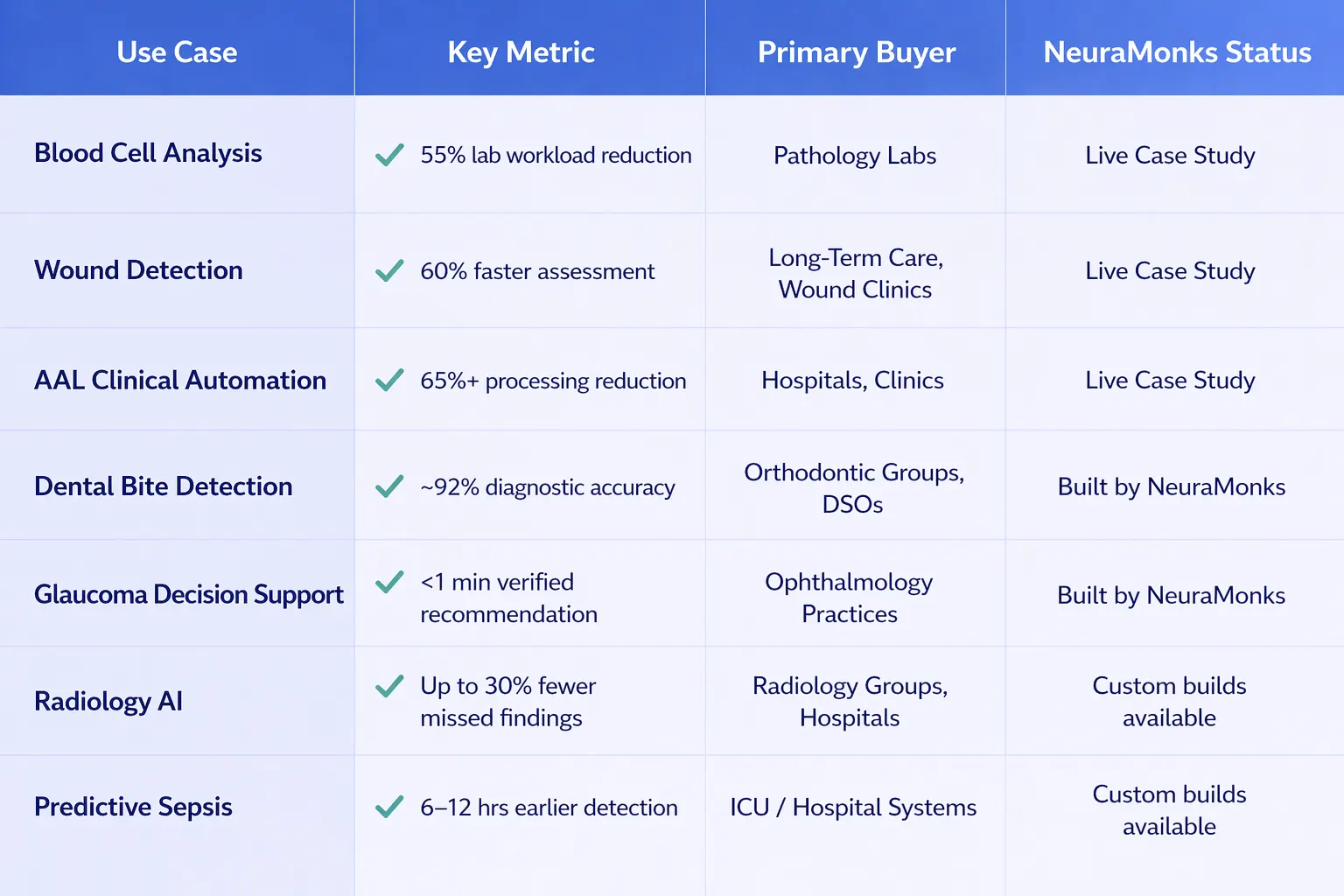
All 7 AI Use Cases: Side-by-Side
The table below maps each AI solution to its primary measurable impact, the clinical buyer, and current NeuraMonks delivery status giving procurement teams a clear evaluation grid.
Your Clinical Problem Has a Measurable AI Answer
NeuraMonks AI Healthcare Solutions are scoped, built, and validated for clinical environments not retrofitted from generic tools. Every engagement starts with a data assessment and a defined success metric.
If your team has a clinical workflow that generates structured data, there is a high probability AI can reduce cost, reduce error, or improve speed — measurably.
Schedule a Clinical AI Scoping Call
45 minutes. Define your use case, assess your data, set success criteria.
Examine Delivered Case Studies
Verified outcomes. Real clinical environments. Exact numbers.
https://www.neuramonks.com/ai-case-study










